Chiari Medicine & Eye Clinic: Providing Comprehensive Eye Care for All Ages
Chiari Medicine & Eye Clinic is a comprehensive eye care clinic that provides a wide range of services for all ages, from routine eye exams to complex surgical procedures. Our team of experienced and board-certified eye doctors and surgeons is dedicated to providing our patients with the best possible care. We offer a wide range of services, including:
- Laser eye surgery
- Cataract surgery
- Glaucoma treatment
- Retinal surgery
- Pediatric eye care
- Ocular disease management

About Me
Chiari Medicine & Eye Clinic is a comprehensive eye care clinic that provides a wide range of services for all ages, from routine eye exams to complex surgical procedures. We are committed to providing our patients with the highest quality care in a comfortable and welcoming environment.
We Are Always Up-to-Date on the Latest Treatments
Our team of experienced and board-certified eye doctors and surgeons is dedicated to providing our patients with the best possible care. We offer a wide range of services, including:
- Laser eye surgery
- Cataract surgery
- Glaucoma treatment
- Retinal surgery
- Pediatric eye care
- Ocular disease management
We also offer a variety of diagnostic services, such as:
- Eye exams
- Visual field testing
- OCT scans
- Tonometry
- Fluorescein angiography

What Services We Are Providing
Here are three of the main services we provide
Laser eye surgery
We offer a variety of laser eye surgery procedures to correct vision problems such as nearsightedness, farsightedness, and astigmatism. Our procedures are minimally invasive and can provide patients with clear, crisp vision for many years to come.

Glaucoma Treatment
Glaucoma is a serious eye disease that can damage the optic nerve and lead to vision loss. We offer a variety of glaucoma treatment options, including medications, surgery, and laser therapy.

Retinal Surgery
The retina is the light-sensitive tissue at the back of the eye. Retinal surgery is used to repair tears, detachments, and other injuries to the retina. We offer a variety of retinal surgery procedures, including vitrectomy, scleral buckle surgery, and laser photocoagulation.
Work Experience
Our team of eye doctors and surgeons have years of experience in providing comprehensive eye care. We are committed to staying up-to-date on the latest advances in eye care technology and techniques.
Our Latest Blogs

An Overview of Laser Eye Surgery: Types and Techniques
Laser eye surgery has revolutionized the field of ophthalmology, offering an effective solution for correcting vision problems. With advancements in technology, various types of laser eye surgery procedures have been developed to address different refractive errors.

The Safety and Efficacy of Modern Laser Eye Surgery Procedures
In recent years, laser eye surgery has become an increasingly popular and effective method for correcting vision problems. This article will explore the safety and efficacy of modern laser eye surgery procedures, as well as the advancements that have been made in this field.

How Laser Eye Surgery Can Correct Refractive Errors
Laser eye surgery has revolutionized the field of ophthalmology by providing an effective solution to correct refractive errors. Understanding these errors is crucial in comprehending how laser eye surgery works to restore clear vision and reduce dependency on glasses or contact lenses.
My Portfolio
We are proud of our work and we want to share it with you. Our portfolio features photos and videos of our patients’ eye care journeys.

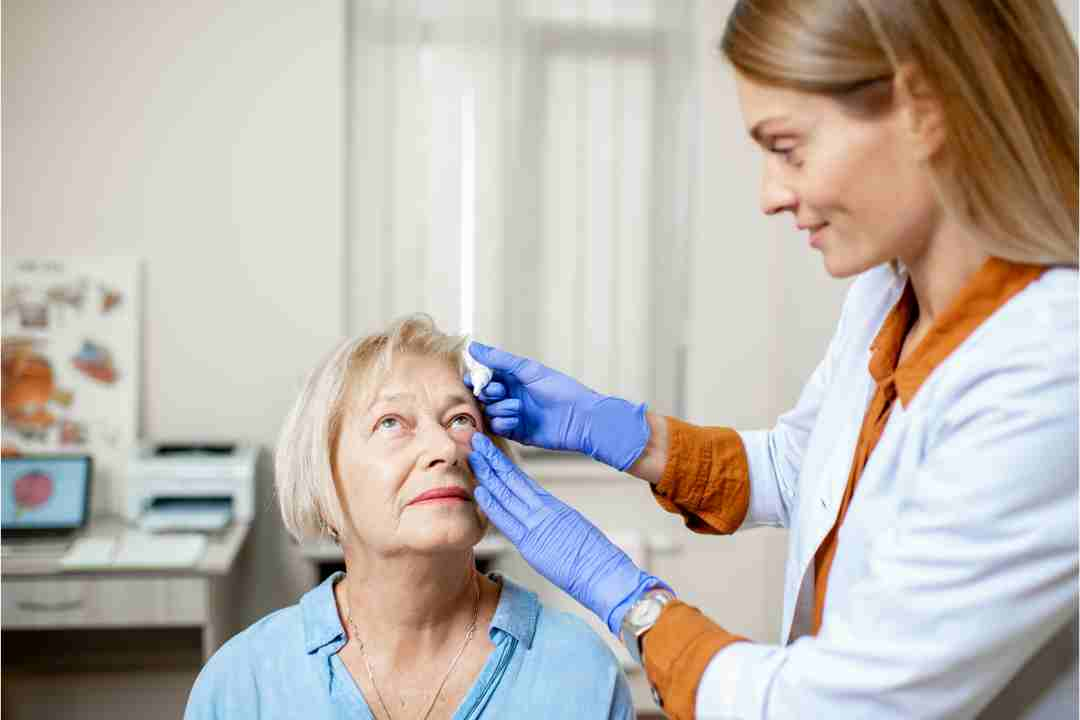
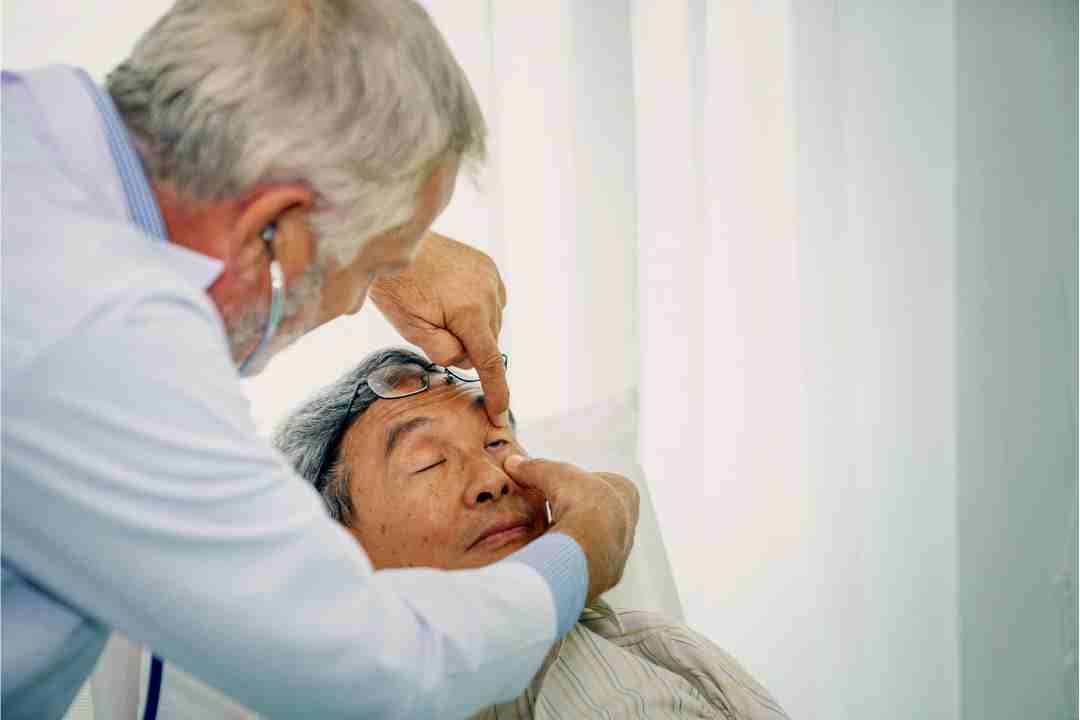







What My Clients Says
We are grateful for the trust that our patients have placed in us. Here are some of the things that our patients have said about us:

“I was so nervous about getting laser eye surgery, but Dr. Smith made me feel so comfortable. The procedure was quick and easy, and I’m so glad I did it!”

“I was diagnosed with glaucoma a few years ago, and I’m so grateful to Dr. Jones for taking such good care of me. I’m confident that I’m getting the best possible treatment.” –

“My daughter had retinal surgery when she was just a baby, and I was so worried about her. But Dr. Brown was amazing. He took the time to explain everything to me, and I knew that my daughter was in good hands.”
Stay In Touch
We hope you will visit our website to learn more about our services and to schedule an appointment.
